|
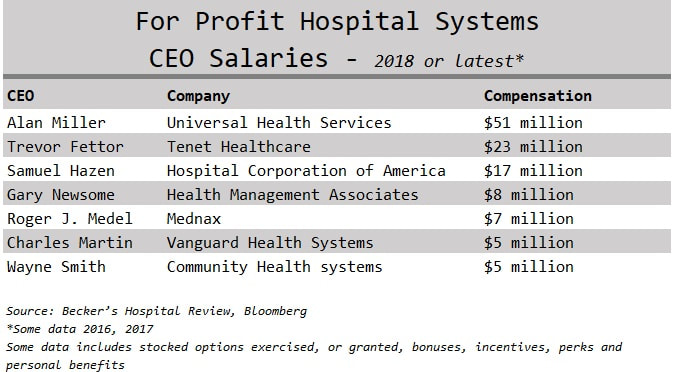
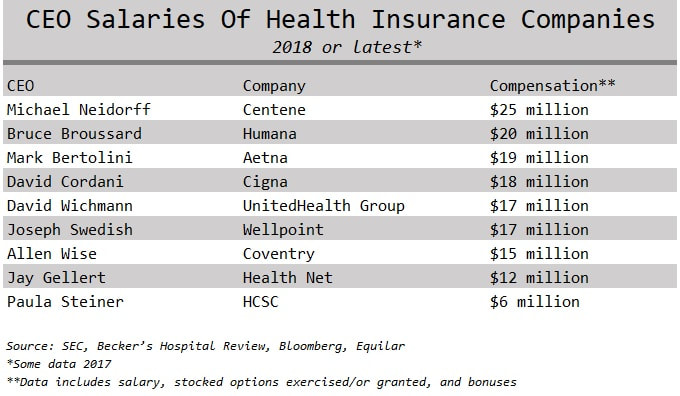
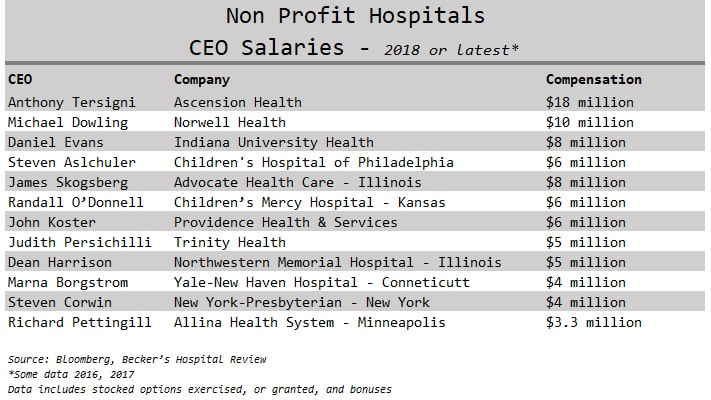
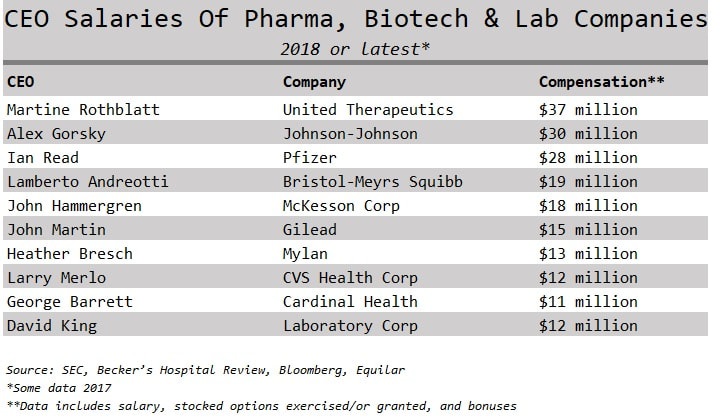
I usually share this quote by writer and blogger Ian Welsh with my students at the beginning of all the healthcare ethics courses I've taught: “Morals are how you treat people you know. Ethics are how you treat people you don’t know.” This is a powerful way to frame the idea of values and how we interact with society. The personal values that we develop as a result of experiencing life creates the foundation for making decisions, guiding behavior, and establishing priorities. Twentieth century philosopher Lawrence Kohlberg devised a theory about how one becomes an ethical person. He called it Stages of Moral Development and concluded that people must go through one stage of development at a time before moving on to the next and that we move through these six stages as we find solutions to the challenges we face in life. Therefore, some people are unable to make certain decisions because of their ethical maturity. Even though someone is an adult physically, they can be morally immature based on the challenges they've been through and how they responded to them. The first two stages in Kohlberg’s theory are called Premoral, or before moral reasoning. Stage three and four are Externally Controlled Morals, or rules of society and culture. Most people remain on these levels. Stage five and six are called Principled Morals, or rules of a higher authority. These include making decisions with the thought that everyone is entitled to common rights. A respect for yourself and tolerance for others requires complex thinking about how you relate with others going beyond what is law. This is believing that all humans have worth and value regardless of their social status. For example, segregation at one time was legal, however, it was unethical and violated a higher law. Only 25% of the population actually gets to these last levels of highest ethical development and maturity. If our experience helps shape our morals, then we need experiences. People without kids do not truly understand people who have kids. The same goes for people with pets, or for people who have lost a child to gun violence. How can we truly feel empathy for somebody in a certain situation until we experience it on our own? Consider the following: How can people who have never been uninsured have empathy for somebody who has lived with no insurance? Can a politician that has never been without insurance advocate for single-payer system that includes all? Will the CEO of an insurance company make decisions to reduce premiums, if she never suffered personal bankruptcy due to health care expenses? Can a man that has never been sexually advanced, groped, molested, or raped develop policies effectively for a woman who has? Yes, it is possible. People with higher ethical maturity levels have the ability to do these things. These types of people, I argue, are the kind of leaders we need making decisions in healthcare. If one wants to buy a Mercedes they can go to a car dealer, pick a color, arrange financing, and have a new car. If one can't afford to buy a Mercedes then maybe they will leave the Mercedes dealer and pursue a Ford Focus or decide to just stick with riding the bus. Either way, you the consumer is in charge of that purchase. Mercedes isn't responsible or under obligation if one cannot secure financing or afford the car with cash. The luxury car maker has no ethical duty. Although healthcare is a business it has very different financial obligations than other industries within our economy. People do not want to purchase cancer treatments, chronic disease remedies, asthma inhalers, or request hip surgery. In the United States health care consumers are not in control of most health purchases outside of the retail market. This comes from the fact that consumers do not manage their healthcare dollars, instead, they send their premiums to an insurance plan that makes most decisions for them. Most health care consumers don't really understand their bills and can't tell you how much their products and services cost them. Health consumers know premiums, deductibles, and co-payments, which are the entry fees into the United States health system. Their choice and role in purchasing is minimal. As a result, we cannot treat healthcare like any other industry in the free market. A healthcare system cannot function without the boundaries of duty and obligation like Mercedes can. However, the reality for Americans is that we are operating outside of those boundaries in a system without duty to the human being. American healthcare is a commodity treated like any other industry within the market economy and is not managed like a human right. In 1948 the United States signed the Universal Declaration of Human Rights which included equal rights to adequate health and health care for nation citizens as a public good. As of today, this makes the United States the only industrialized and developed nation that hasn't secured health care as a public right for its citizens. Since someone else takes care of our healthcare dollars, and these healthcare resources are limited, using them must be done in a responsible way. The balance of profit and social justice is a true dilemma in our healthcare system, but is it not impossible to balance that scale. If leaders of an organization are motivated by money, it can deter the mission of caring for the sick and injured, promoting prevention, and keeping people healthy and happy. Fiscal responsibility is a duty to be responsible and accountable with money, especially someone else's, and is a marriage of numbers and values. Therefore, an organization's financial statement is their ethical statement. This is because what an organization prioritizes and spends their money on defines what's important to them. One of the biggest issues we have in the United States healthcare system is not having enough money for health care, but it is how that money is spent. Check out the salaries below of top health industry executives and consider what their organizations prioritize and what their values are: Nearly all large healthcare organizations make their top executives extremely rich. A perverse incentive to profit off the sick. Sarah Anderson, Global Economy Director at the Institute for Policy Studies said "If executives are loaded up with stock options and other types of equity-based pay, they have a personal incentive to boost shares prices by whatever means necessary.” One top earner is CEO Martine Rothblatt of the pharmaceutical company United Therapeutics who took home $37 million in 2018. United Therapeutics makes drugs to treat high blood pressure and for pediatrics with high-risk cancers. For comparison purposes, Seema Verma the CMS administrator who oversees Medicaid and Medicare is given $165,000 in salary paid by tax dollars. If CMS administrators were getting paid $5 million dollars with tax money there would be upheaval about how our tax money is spent. How come we don’t question how our other healthcare dollars are spent? Where do you think these executives fall within Kohlberg’s ethical maturity levels? In the current environment of 30 million people uninsured, and millions of others having high deductibles they can't afford, do you think it's acceptable for these types of compensations? Is it justified or fair that health CEOs took home 11% more of our money on average every year since 2010 according to an Axios analysis. What are the priorities of these executives when they take such high salaries? Is this fiscally responsible with our limited shared resources? Welcome to the executive compensation problem that exists in the United States. Other countries don't seem to have the same CEO compensation problem that we do. How big of an ego does the United States have? Kohlberg’s Stages of Moral Development theory notes that it is possible for people to be unable to make certain decisions because of their ethical maturity. This provides an explanation for how healthcare executives can take home salaries of multi-millions of dollars amidst all the challenges the health system currently has; people are unable to afford to get a necessary surgery, procedure, or medication because their deductibles are too high, every six minutes a patient dies in an American hospital from a hospital-acquired infection, preventable hospital errors persist as the number three killer in the US–third only to heart disease and cancer, and on average a hospital patient is subject to one medication error per day. Large corporations and CEOs will argue that these wages are necessary to attract the best and brightest executives to the healthcare industry. How is it that our executive health leaders think they deserve such pay when our system is in shambles? For most other people in the corporate world bonuses and raises are based on performance and hitting targets and goals. I can't imagine we are hitting targets and goals with the current state of our health system. Or maybe the targets and goals should change? CEO Wayne Smith of Community Health Systems had received $16 million dollars in total compensation yet recently settled a lawsuit alleging false billing and kickback allegations, both federal crimes. If our system was booming with better health outcomes, affordable coverage, less fraud, and no uninsured, then perhaps it would be justified to have executives taking such high pay. Further, if we treat healthcare as a right, or like most countries do as any other public service like the library or police, then our current system functions without morals (or pre-moral stage one-two) also known as immoral. If leaders in healthcare had a stage five or six ethical maturity level (principled morals of a higher authority) do you think they would take salaries such as these? It is hard to argue that these executive leaders are ethically mature.
Healthcare isn’t Pepsi, Coach, Kellogg, Hilton, Koehler, or Mercedes. People don't need to drink Pepsi, wear Coach bags, eat corn flakes, or stay at hotels to survive, but they do need access to healthcare for optimal health and wellness. Leaders in healthcare must have different values than leaders in other industries within the shared economy because of this striking truth. To put this into perspective let's examine the scenarios of CEOs taking a pay cut:
The opportunities are endless in what health executives can do with our health dollars instead of high salaries for themselves and the rest of their executive c-suite team: lowering of deductibles and copayments, adding additional coverage such as functional medicine, holistic practitioners, more psychotherapy sessions, coverage for massages, provide free or low -cost services/programs/screenings, or increases in salaries for workers. What is it that organizations are willing to give up to take on a large multi-million-dollar salaries for their executive teams? Again, an organization’s financial statement is their ethics statement. Do you think they are acting with social and fiscal responsibility? Specifically for pharmaceutical companies where executive compensation is higher than most health sectors, consumers do not directly feel the pain of the high costs of prescription drugs. This is because the costs are in co-pays which are set fees we can expect. These high costs are filtered through the system and hidden as higher premiums and deductibles because our insurance companies pay the rest of the bill for us with our premium dollars. We are not only paying for the drug itself, but also supporting a $66 million-dollar salary for its CEO. In 2017 healthcare reporter Bob Herman published an analysis of the salaries of over one-hundred CEOs of seventy of the largest U.S. healthcare companies since 2010 based on corporate financial filings and cumulatively these CEOs have earned $9.8 billion. Imagine the magnitude of those dollars and how they could be spent differently within our system. The Institute for Policy Studies note that $75 million is the equivalent of the cost of dental insurance for 250,000 Americans or the average annual health insurance plan deductible for 24,000 people. That is just a small fraction of that $9.8 billion. Even more, consider the cumulative cost of the rest of the c-suite that get similar salaries: CFO, CEO COO, CIO. An analysis done by Modern Healthcare noted that one company alone, Health Care Service Corp., the Blue Cross and Blue Shield insurer in five states, paid the top ten executives cumulatively $56.7 million in 2015. There are several familiar guiding principles of healthcare ethics such as doing no harm, preserving life, being discreet, upholding justice, and respecting autonomy. Health leaders will never be given enough resources to satisfy all the demands placed upon them by a community, but they can turn to the guiding principle of justice to help them distribute their yearly budgets ethically. Justice refers to fairness and equality and stems from a rather simple but complex ethical concept called the Philosophy of Individual Worth. It is a duty and moral obligation for health systems to give the same treatment to everyone regardless of one’s circumstances. Leaders in healthcare have a duty to go beyond personal feelings and honor the individual’s worth. I mean, really, we want the same don’t we—for people to respect our needs, what we want, and believe? But this is hard to do and as a result, leaders in healthcare must have this skill, which I argue is only possible by some with higher ethical maturity. Justice is also the fair distribution of benefits offered by a society and includes the fair distribution of its burdens as well. Society suffers injustice when not everyone gets to share in the benefits and when distributions of resources are not equal. In healthcare this creates an environment where health equity is compromised and health disparities shade society with injustice, which is the unfortunate reality in the United States. Since we live in a healthcare system where someone else takes care of our healthcare dollars, the concept of good financial stewardship and the duty to be fiscally responsible with limited healthcare resources is supported by the ethical principle of justice. Award-winning 20th century philosopher John Rawls was interested in what makes a just and moral society. He formulized a hypothetical theory where people are equal to each other and all humans have worth in the Original Position and if we take a Veil of Ignorance with each other a social contract would develop that secures basic rights for everyone and protect those in all positions of society. His theory goes on to say that the advantaged have a responsibility to the disadvantage. Those that are disadvantaged could include those in poverty, ones with chronic disease that affect the quality of life, the disabled, etc.. Therefore, in the end, it is in our ultimate best interest to do this because everyone has the potential to be in the lesser position (loss of job, health, etc). John Rawls said “a just society is a society that if you knew everything about it, you'd be willing to enter it in a random place.” Consider that powerful thought: are you willing to be born into a low-income, black family in Chicago? Statistically this population has the highest health disparities in the country, and as a result, end up in unhealthy situations that produce a symptom of another statistic; highest homicide rate. At the core of Rawls theory is that no matter what our circumstance, environment, or influence, we are human, and all human interests must be observed to truly live in a moral, ethical, and just society. This is not what our reality is today. Especially not in our health system. If we want people to be tolerant of our ideals, we must be tolerant of others. This is why the balancing scales are often the symbol used for justice. Only one set of ideals getting priority does not work. Executive compensation metrics are a powerful reflection of the priorities of an institution. While the general population complains about, and suffers from, the ever rising healthcare costs, no one is championing efforts for fiscal responsibility and transparency of the spending of our shared resources by executive leaders in healthcare. Instead, the general American population is unknowingly supporting executive leaders becoming very rich off of the sick and our limited healthcare dollars. We have evidence popping up every day in our society that the status quo is not working. Just as health leaders reduce the numbers of nurses on the floor that care for patients in order to save health dollars, maybe we should consider eliminating a few million dollars of executive pay instead. What do you think will positively impact patients more: fewer nurses or less executive pay? According to a JAMA study, there is no link between CEO pay and hospital quality indicators such as re-admission rates, mortality rates, or community outreach programs. In other words, a highly paid CEO will not necessarily increase the performance of a hospital and the outcomes of patients. Its unsettling that CEOs at hospitals with high mortality rates are being paid just as much, or sometimes more, than those at hospitals with lower rates of mortality. Physician compensation is increasingly being tied to quality measures and I argue that executives should be treated the same given that they have a fiduciary and ethical responsibility to represent the welfare of the community in which the serve. An analysis by Kaiser Health News found it was more common for executive bonuses to be tied to boosting volume rather than increasing quality, which unfortunately sets up an environment where the incentives are to keep people returning to the hospital, not preventing them from needing to be readmitted. With that, I am calling for policymakers, tax payers, and health consumers to consider new public policy to tackle the injustice of excessive executive pay that exists in the American health system. I am proposing a professional consideration of placing caps and limits on executive compensation in these fields. This is argued based on the fact that healthcare is something every human needs, and is an industry that all is born into, lives, and dies in, it simply cannot be employed in the same manner as a company that sells running shoes. The recommended process for determining the appropriate compensation usually is to conduct a review of what similarly-sized organizations in the same geography offer their senior leaders. However, since healthcare is not like any other industry due to its ethical duties and obligations, the same process simply cannot apply. A new way of calculating executive compensation must be developed so that precious and limited healthcare resources can be distributed fairly and used effectively. Until that happens, I am calling for health executives to make a progressive move and donate their excessive compensations back into the system. Does anyone have the guts? I believe wholeheartedly that ethically mature leaders in healthcare exist that are capable of making major healthcare business decisions without the multi-million-dollar salary to prove their worth and competency. The present chaos that exist within our healthcare system shows that the current model of excessive executive compensation is not working and immoral. Begin to take power back and become an informed health consumer. Share this with somebody you care about.
1 Comment
2/6/2022 09:57:58 pm
<b><a href="https://www.onegeneric.com/product/buy-sildenafil-100-mg-capsule-online-fildena-super-active-capsule">buy fildena super active online</a></b> taking it with a heavy or high-fat meal can slow the time it takes it to start working by about an hour. Fatty foods might also increase the risk of stomach upset. A full stomach may also make sexual activity uncomfortable.
Reply
Leave a Reply. |
Kat LahrResearcher, Writer, Educator, Reformer & Believer of Health Care as a Right Archives
April 2020
|
|
CREATING AWARENESS IN
HEALTH CONSUMERS |
TC Publishing |
|




 RSS Feed
RSS Feed

